WATCHMAN: A better way to reduce stroke risk for some AFib patients
- Category: General, Cardiology
- Posted On:
- Written By: Boulder Community Health

AFib raises a person's risk for stroke by 500% (according to the National Stroke Association), since AFib can cause a blood clot that leads to a stroke.
“Once you have the AFib diagnosis, the goal is to consider two things: one, manage the AFib itself and the other, reduce the risk of stroke,” says Boulder Heart structural interventional cardiologist Chirag Chauhan, MD, MS, FACC, FSCAI.
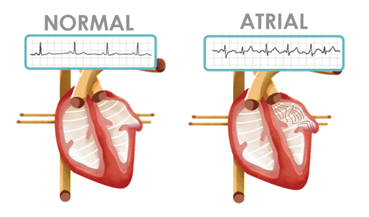
What is atrial fibrillation?
- Atria: two small upper chambers
- Ventricles: two larger lower chambers
Together, the chambers pump blood to and from other parts of the body. AFib is a heart condition that causes the upper chambers of your heart to beat irregularly and in a chaotic rhythm due to “disorganized electrical signals in the heart,” according to Dr. Chauhan. The rhythm, which can be fast or slow heart beats, also doesn’t communicate normally with the bottom ventricles, says Dr. Chauhan.
The risk of AFib increases with age, especially for those 60 and older. While AFib is a common cardiac condition, it’s a growing concern, as up to 12 million Americans are expected to be affected by 2030. By 2050, that number is expected to rise to 16 million. The five million people currently dealing with AFib will share that it creates a significant impact on quality of life and it takes time to determine the right treatment options.
Not every “irregular heart rhythm” is AFib. The AFib rhythm can be short-lasting or come and go with unpredictable episodes.
Once a cardiology provider has diagnosed you with AFib and determined your type of AFib, you and your physician can focus on your risks and the best treatment strategy.
AFib & the risk for complications
These include:
- Blood clots: The irregular heart rhythm can cause blood to pool and form clots in an area of your heart called the Left Atrial Appendage (LAA)—a small sac in the left atrium (the top left heart chamber).
- Stroke: People with AFib may be at greater risk for stroke—up to five times higher—than people with normal heart rhythms. AFib can significantly decrease the heart’s pumping capacity which increases the risk of clots forming. If a blood clot forms in the LAA, it can escape and travel to the brain to cause a stroke.
- Heart failure: If AFib continues over a long period of time, the decreased efficiency of the heart from the top chambers to the bottom chambers can lead to heart failure, with fluid pooling in the lungs, legs or other areas.
“Approximately 1 in 3 people with AFib will have a stroke in their lifetime, and AFib-related strokes are more frequently fatal and disabling,” says Boulder Heart structural interventional cardiologist Srinivas Iyengar, MD.
AFib treatment options
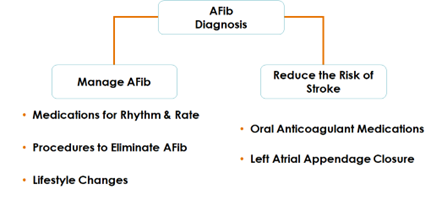
The management of AFib includes medications for rate or rhythm control, lifestyle changes (regular exercise, a heart-healthy diet, not smoking and limiting alcohol/caffeine), and AFib procedures such as cardioversion (shocking the heart out of AFib back to a normal rhythm) or ablation (burning tissue to prevent reoccurrences of AFib).
To reduce the risk of stroke, patients can depend on on oral anticoagulation medications (also known as blood thinners) or Left Atrial Appendage Closure (LAAC) Devices, such as WATCHMAN. Blood-thinning medications like Eliquis, Xarelto and Pradaxa are the most common treatment for protecting AFib patients from stroke. These clot-preventing medications, which patients can safely take for years, can greatly reduce stroke risk if patients take them properly (no skipped doses) and do not experience adverse side effects.
“When considering treatment options, I will weigh in about the patient’s risk of a stroke. We look at the CHA2DS2-VASc Score—a scoring system to help determine risk of stroke. At the same time, we look at risk for bleeding—the HAS-BLED Score,” says Dr. Chauhan.
The anti-coagulant medications do come with an increased risk of bleeding (fatigue, diarrhea and others have also been reported) and adverse consequences for taking the medication intermittently, and that’s why patients may want to seek out a procedural option.
“A lot of my patients will say, ‘I tried the medication. I don’t like it.’ Or I read about the medication. I don’t want to take it.’ Or I don’t have that much AFib, I don’t really need it,’” says Dr. Iyengar. “In reality, [the number of] patients taking these medications [correctly] is well below 80%. And if you [only] take this medication occasionally, sometimes, not all the time, you can increase your stroke rate up by 64%.”
Left Atrial Appendage Closure (LAAC) with WATCHMAN
Closing the LAA is an effective way to reduce stroke risk in people with AFib that is not caused by heart valve problems.
The most implanted LAAC device in the United States is the WATCHMAN Implant—designed to close off the left atrial appendage, the formation site of most stroke-causing blood clots.
Patients turn to the WATCHMAN because they’ve experienced bleeding while taking blood thinners or have a lifestyle, job, fall risk or health condition that puts them at risk for bleeding.
“For certain individuals, there are barriers to taking a blood thinner, including dangerous interactions with other medications, dietary restrictions, high prescription costs, and concerns about bruising or excessive bleeding from an injury,” says Dr. Iyengar.
The Boulder Heart team is proud to offer patients the latest in WATCHMAN technology—the WATCHMAN FLX Pro™ Device—a next-generation, updated design with three new features to advance performance and safety and ensure the best long-term outcomes. The device is available in six sizes (20, 24, 27, 31, 35 and 40mm) to accommodate various, complicated left atrial appendage (LAA) anatomies.
“There are some anatomies that do not lend itself to implantation of a WATCHMAN device, and those anatomies may be better served with a different type of device,” says cardiac electrophysiologist Oussama Lawand, MD, FHRS.
BCH also utilizes the WATCHMAN TruSteer™ Access System—a complement to the WATCHMAN FLX Pro™—which supports steering and a greater range of motion to position the WATCHMAN implant for more complicated anatomies.
Why might a patient consider WATCHMAN?
- The WATCHMAN Implant is FDA-approved and has been studied for more than 20 years, with a proven safety record. Worldwide, more than 200,000 people have received the WATCHMAN Implant.
- WATCHMAN is a one-time minimally invasive procedure (lasting about an hour) under general anesthesia that may reduce stroke risk for a lifetime. It’s an effective stroke risk alternative to a lifetime of blood thinner worries in certain populations for those with AFib not caused by heart valve problems (NV AF).
- The Implant—which is permanent and about the size of a quarter—is made from very light and compact materials commonly used in other medical implants.
- May eliminate long-term oral anticoagulant use and reduce the long-term risk of bleeding associated with anti-coagulants use.
- Does not require traditional open-heart surgery and the device cannot be seen outside the body.
- Some patients who have significant AFib symptoms and high risk for bleeding are candidates for an AFib ablation and a WATCHMAN device. Your cardiologist will discuss with you a unified strategy to address AFib rhythm issues and LAAO stroke risk in one single procedure. These procedures are performed by cardiac electrophysiologistDr. Lawand.
Weighing the risks of WATCHMAN
According to Dr. Iyengar, there is no “perfect” therapy to completely eliminate stroke risk. The decision to move forward with a WATCHMAN implant, he says, should involve all the major pros and cons while debating procedure vs medication. The choice is not one-size-fits-all, and he asks his patients to be honest about their reasonings for not wanting to take blood thinners.
The results of a landmark WATCHMAN study (3,000 patients, randomized 1:1, over three years) were recently released at the American College of Cardiology national meeting. The 2026 CHAMPION-AF trial results indicate that the WATCHMAN FLX™ Left Atrial Appendage Closure (LAAC) device is a safe and effective first-line alternative to non-vitamin K oral anticoagulants (NOACs) for non-valvular atrial fibrillation patients. The study found the device significantly reduces bleeding risk compared to medication while providing similar, effective stroke protection.
The trial showed less than one percent (0.6) percent of serious adverse events. Overall, the study identified 17 more strokes in the WATCHMAN patients and four fewer episodes of major bleeding with WATCHMAN.
Schedule an appointment
To find out if you’re a candidate for WATCHMAN, schedule a consultation with Dr. Iyengar or Dr. Chauhan. To learn more about AFib ablation, connect with Dr. Lawand. Call Boulder Heart at 303-442-2395.
Watch the recent WATCHMAN lecture, presented by Drs. Chauhan, Iyengar and Lawand, here.