Dr. Robert Shapiro on managing your cholesterol
- Category: General, Cardiology, Primary Care
- Posted On:
- Written By: Boulder Community Health

Eighty-six million American adults have high cholesterol. However, because it has no symptoms, only 55% of those who could benefit from cholesterol medication take it. And, in the last five years, 33% of adults haven’t taken the simple blood test that quickly diagnoses cholesterol levels.
High cholesterol can lead to heart attacks and strokes; fortunately, there are simple and practical steps for managing and lowering cholesterol levels.
As a part of the BCH educational lecture series, board-certified cardiologist Robert Shapiro, MD, FACC, of Boulder Heart at Erie and Boulder Heart at Longmont spoke on a topic he is passionate about: managing our cholesterol. As an interventional cardiologist, Dr. Shapiro especially enjoys educating his patients about their health options so that they can continue to enjoy life to its fullest. In his presentation, Dr. Shapiro provided information on diet and lifestyle changes, as well as medications, that reduce cholesterol levels and the risk of heart attack and stroke.
______________________________________________________________________________
Watch: “Managing Your Cholesterol"
______________________________________________________________________________
Let’s talk about what cholesterol is
Dr. Shapiro described cholesterol as “a waxy substance produced in the liver and found in all our body’s cells.” He further explained that cholesterol does have important functions. “Our bodies need some cholesterol to make hormones, vitamin D and substances that help us digest foods.” Because our bodies do produce all the blood cholesterol we need, it’s recommended we eat as little dietary cholesterol as possible.
Why worry?
High cholesterol can lead to a buildup called “plaque” on the walls of our arteries. Dr. Shapiro said, “From my perspective, I worry about cholesterol because as an interventional cardiologist, I want to prevent patients from experiencing heart disease. Over time as plaque builds up, our arteries narrow, and this can cause these deposits to suddenly break and form a clot that causes a heart attack or stroke.”
Good vs. bad cholesterol
A standard lipid panel is a blood test that measures our lipids, the fats and fatty substances used as energy for our bodies. The panel results are a summation of high-density lipoprotein (HDL), low-density lipoprotein (LDL) and triglycerides.
- High-density lipoproteins (HDL)—are the “good” cholesterol that at a healthy level protects against heart attack and stroke. “HDLs can be cardioprotective,” said Dr. Shapiro, explaining, “HDLs actually take cholesterol from the arterial walls and blood and return it back to the liver to be recycled.”
- Low-density lipoproteins (LDL)—are the “bad” cholesterol. “LDLs contribute to fatty buildup in the arteries and increases the risk of heart attack and stroke,” said Dr. Shapiro.
- Triglycerides—are the most common type of fat in our bodies. “High triglycerides can be a sign of other conditions that increase our risk for heart attack and stroke. Extremely high triglycerides can cause pancreatitis,” explained Dr. Shapiro.
How often you get a lipid panel done depends on your age, risk factors and family history of high blood cholesterol or cardiovascular diseases. The National Heart Lung and Blood Institute (NHLBI) recommends the following:
- Age 19 or younger: Screening begins at ages 9 to 11 and should be repeated every 5 years. Screening may be performed as early as age 2 if there is a family history of high blood cholesterol, heart attack, or stroke.
- Age 20 to 65: Younger adults should be screened every 5 years. Men ages 45 to 65 and women ages 55 to 65 should be screened every 1 to 2 years.
- Older than 65: Older adults should be screened every year.
Advanced lipid testing is usually performed in addition to a standard lipid panel for those with a family history of cardiovascular disease that can’t be controlled with a healthy diet and exercise. Two commonly used advanced lipid tests are apolipoprotein B (apoB) and LDL particle number (LDL-P).
Living a heart-healthy lifestyle can prevent high cholesterol
Dr. Shapiro emphasized that following a healthy lifestyle is the first defense against high cholesterol.
- Exercise—150 minutes per week to lower LDLs and triglycerides and raise HDLs.
- Lose weight—a weight loss of 3% to 5% for those categorized as obese can increase HDLs and decrease LDLs.
- Reduce stress—stress can lead to higher cholesterol levels.
Healthy diets that lower cholesterol include eating:
- fruits and vegetables,
- nuts such as walnuts and almonds,
- whole grains-oats and barley,
- lean vegetables and/or animal protein,
- lean, oily fish and skinless poultry, and
- green tea.
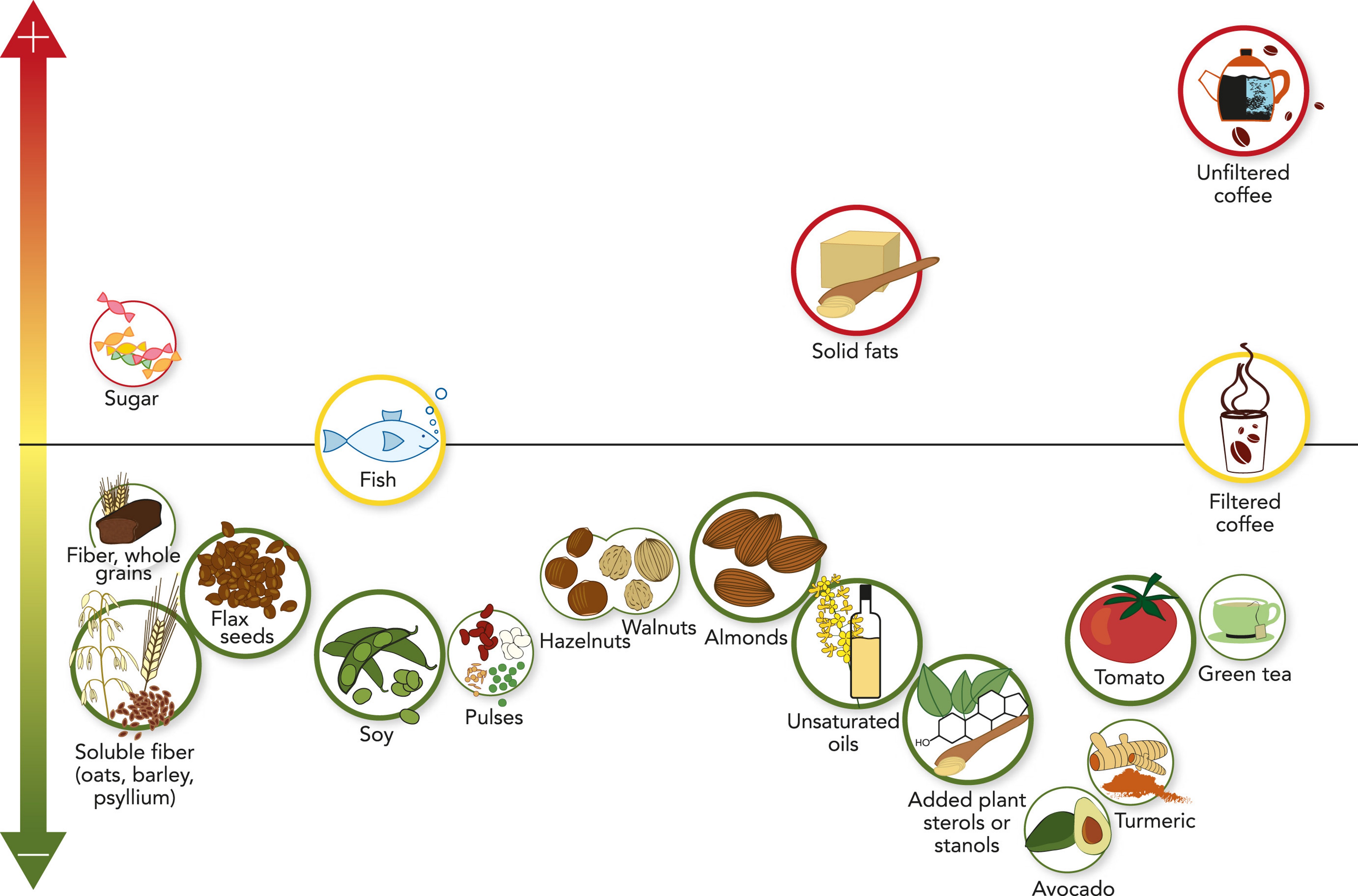
![]()
Healthy lifestyle diets include:
- Mediterranean diet
- DASH diet
- Plant-based (vegetarian/vegan) diets
- Flexitarian diets—mostly vegetarian with some lean meats and/or fish
- Portfolio diet
- Plant proteins, nuts, viscous fiber, phytosterols and plant monounsaturated fats
Foods to avoid that increase cholesterol include:
- sugar,
- sweetened beverages,
- refined carbohydrates—simple sugar, white bread, pasta,
- red meat, like beef, pork and lamb, as well as processed meats like sausage,
- butter,
- tropical oils such as palm and coconut oil,
- trans fats found in fried foods, commercial baked goods, processed foods and margarine and
- unfiltered coffee.
When are medications appropriate?
“Most cholesterol medications lower cholesterol with few side effects. Even with effective medication, however, it’s still important to follow a healthy diet and get regular exercise,” said Dr. Shapiro.
Dr. Shapiro recommends “discussing cholesterol medications with your health care provider if you’re 20 to 39 and have a strong family history of cardiovascular disease or if your bad cholesterol is greater than 160. Patients with bad cholesterol of greater than 190 should be on a high intensity statin and those who are diabetic and age 40 to 75 should be on a moderate to high-intensity statin therapy.”
There are multiple factors that your provider and you will want to consider when determining the most appropriate treatment, these include:
- age,
- risk factors and
- your history of cardiovascular events.
Statins
“Statins are oral medications and the most commonly prescribed cholesterol medications,” said Dr. Shapiro. They reduce the amount of cholesterol made by the liver and help the liver remove cholesterol already in the blood. He added, “These are safe, well-tolerated medications. Generally, everyone who’s had a heart attack should be on a high-intensity statin, if they can tolerate it. We have an enormous amount of reliable data indicating that statins lower the risk of having another heart attack or stroke.”
Ezetimibe
Ezetimibe is often prescribed for patients who cannot take statins. It helps stop the body from taking in cholesterol from food and can lower cholesterol levels within two weeks.
PCSK9 Inhibitors
The PCSK9 inhibitor is administered as an injection every two weeks. It results in the drastic reduction of LDLs but can be very expensive.
Dr. Shapiro said, “It’s important to remember that cholesterol management can be simple but may require a multi-pronged approach that includes a healthy diet, exercise and potentially medication.”
Schedule an appointment
Call 720-853-3032 if you have any questions or to schedule an appointment with Robert Shapiro, MD, FACC, at Boulder Heart at Erie or Boulder Heart at Longmont.
Click here to view/download a PDF of slides shown during the lecture.
Want to receive notification of special events and lectures?